
Introduction
Healthcare organizations are navigating a crisis on multiple fronts: over 1 million RN retirements projected by 2030, a national RN vacancy rate of 9.6%, and post-pandemic burnout affecting 60% of acute care nurses.
Escalating patient safety expectations and relentless cost pressures compound these numbers — leaving hospitals short-staffed, overburdened, and increasingly vulnerable to clinical errors.
Employee engagement sits at the center of all these challenges. Yet despite widespread discussion in healthcare, organizations often reduce its value to survey scores or retention metrics. That framing misses the point. Disengaged employees don't just perform poorly — they actively harm patients, erode safety culture, and drain organizational resources.
What follows is the measurable evidence for treating engagement not as an HR initiative, but as a core driver of patient outcomes, safety culture, and long-term organizational health.
TL;DR
- Employee engagement is how committed clinical and non-clinical staff are to giving their best effort
- Engaged healthcare teams outperform disengaged peers on patient experience, safety reporting, and retention
- Disengagement causes real damage: more errors, higher burnout, costly turnover, and declining patient satisfaction
- The root cause is behavioral — environments that don't reinforce excellent care
- Fixing it requires evidence-based behavioral methods, not one-time surveys or wellness programs
What Is Employee Engagement in Healthcare?
Employee engagement in healthcare is the extent to which staff are involved in, enthusiastic about, and committed to their work and their organization's mission. More importantly, it's how that commitment shows up in day-to-day behavior—at the bedside, in care teams, and under pressure.
Engagement becomes operationally visible in observable behaviors: how nurses interact with patients during shift changes, how physicians communicate critical information during handoffs, how support staff follow infection control protocols, and how leaders model organizational values when resources are constrained.
Engagement is a means to an outcome, not an end in itself. The goal is the downstream results that engaged behavior produces: safer care, better patient experiences, and lower turnover.
When staff are engaged, they give what behavioral scientists call Discretionary Effort (the gap between the minimum required and the maximum they're capable of). That difference separates adequate care from exceptional care.
According to Press Ganey's 2024 healthcare workforce analysis, approximately 69% of healthcare workers surveyed (2.2 million employees) are engaged or highly engaged. That means nearly one-third of the healthcare workforce is not engaged—a gap with measurable consequences.
Key Advantages of Employee Engagement in Healthcare
The three advantages below are grounded in measurable operational outcomes—not abstract ideals. Each directly affects the metrics healthcare leaders are held accountable for: HCAHPS scores, safety incident rates, and workforce costs.
Advantage 1: Higher Patient Experience and Clinical Quality Scores
Engaged employees make the behavioral difference patients actually notice. They take extra time to explain a diagnosis, follow up on comfort needs, and advocate for the patient's concerns. Disengaged staff withhold these behaviors.
Engaged staff give Discretionary Effort — effort beyond the minimum — and it shows up in clinical interactions that patients remember and report. Research indicates engaged employees perform approximately 20% better than their colleagues, and highly engaged healthcare organizations are 3x more likely to be top performers in patient experience.
This has direct cost and quality consequences:
- HCAHPS scores affect CMS reimbursement under the Hospital Value-Based Purchasing Program, which redistributes 2% of Medicare payments ($1.9 billion in FY2020) based on quality performance
- Patient satisfaction influences referrals, reputation, and revenue
- For every 1% increase in employee turnover, patient experience scores drop an average of 2 percentile ranks
Conversely, burnout erodes quality. A meta-analysis of 85 studies covering 288,581 nurses found nurse burnout is associated with lower patient satisfaction, lower nurse-assessed quality of care, and significantly more missed care or care left undone.
Quality metrics affected:
- HCAHPS scores
- Patient satisfaction percentile rankings
- "Likelihood to Recommend" rates
- Readmission rates
- Care protocol adherence
The engagement-to-patient-experience link is most acute in high-volume, high-acuity settings — ICUs, emergency departments, and post-acute rehab — where emotional labor and attentiveness are continuously demanded from staff.
Advantage 2: Stronger Safety Culture and Fewer Adverse Events
A disengaged workforce is a safety risk. Staff who feel unsupported or undervalued are less likely to speak up about near-misses, report errors, or flag unsafe conditions. Engaged employees actively protect patients and each other.
Psychological safety — a key dimension of engagement — directly determines whether staff report incidents or stay silent. A meta-analysis of 14 studies (n=30,490) found:
- Overall correlation between staff engagement and patient safety outcomes: r = 0.22
- Engagement and errors/adverse events: r = -0.20 (higher engagement = fewer errors)
- In one large study, 58% of highly engaged employees scored in the top quartile of patient safety culture; only 3% scored in the lowest quartile
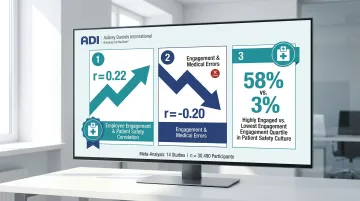
The JAMA Network analysis found nurse burnout associated with worse safety culture, more medication errors, more adverse events, and more patient falls. Emotional exhaustion had the strongest negative effect on patient safety.
The financial and regulatory stakes are significant: unreported near-misses lead to preventable adverse events, malpractice exposure, and CMS penalties. Under the Hospital-Acquired Condition Reduction Program, hospitals in the worst-performing quartile receive a 1% payment reduction on all Medicare reimbursements.
Safety metrics affected:
- Safety incident reporting rates
- Patient harm events
- Medication error rates
- Hand hygiene compliance
- Joint Commission survey outcomes
Safety culture engagement is especially critical in high-stakes units — surgical, pharmacy, labor and delivery — where protocol adherence and communication failures have direct patient mortality implications.
Advantage 3: Reduced Turnover and Lower Workforce Costs
Engaged employees stay. That compounds in healthcare, where the cost of replacing a single RN averages $61,110 (ranging from $49,500 to $72,700 in 2024), and vacancy rates cascade into agency staffing expenses.
Engagement reduces the intent-to-leave cycle. Employees who feel recognized, purposeful, and supported in growth are far less likely to leave. According to Press Ganey's 2025 data:
- Disengaged healthcare employees are 1.7x more likely to leave their positions
- RNs with low teamwork scores are 1.53x more likely to exit
- Weak leader relationships increase departure likelihood by 44%
The numbers reflect this directly:
- Each 1% change in RN turnover represents approximately $289,000 in costs or savings per hospital per year
- Average annual hospital cost of RN turnover: approximately $5.19 million
- Travel nursing revenue surged from $8.7 billion in 2019 to $44.6 billion in 2022 — a 5x increase driven by vacancies
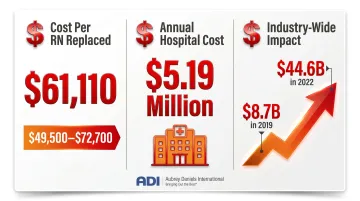
High turnover taxes remaining staff (increasing burnout), destabilizes care continuity for patients, and drives up operating costs through reliance on agency and contract labor.
Workforce metrics affected:
- Voluntary turnover rate
- Vacancy rates
- Agency/contract labor spend
- Time-to-fill open positions
- 90-day new hire retention
Retention ROI is highest in organizations already relying on travel nursing or facing active nursing shortages — where the compounding cost of disengagement shows up directly on the balance sheet.
What Happens When Employee Engagement Is Ignored
The operational reality of a disengaged healthcare workforce: staff who meet the minimum, avoid discretionary effort, and emotionally check out. This creates a care environment that feels transactional to patients and demoralizing to peers who remain committed.
Concrete consequences accumulate over time:
- Patient complaints and declining HCAHPS scores as attentiveness and communication quality drop
- Higher near-miss and adverse event rates as disengaged employees underreport or skip protocol steps
- Accelerating turnover as disengaged employees either leave or pull down the engagement of those around them—active disengagement is contagious; research shows turnover emotional contagion nearly triples the effect of role overload on turnover intent
- Rising labor costs from agency staffing, overtime, and constant recruiting and onboarding cycles
- Leadership credibility erosion when staff see engagement initiatives that are superficial or inconsistently applied

The financial scale of this problem is hard to ignore. Globally, disengaged and actively disengaged employees cost $10 trillion in lost productivity — roughly 9% of global GDP. In healthcare specifically, turnover from non-engaged employees costs an average of $25 million per organization per year.
Those costs don't accumulate without a cause — and increasingly, the cause starts at the top. Leader engagement has dropped 3.7% over the past three years, making leaders one of the only workforce segments that hasn't reversed COVID-induced engagement declines. Disengaged leaders don't just underperform — they model the disengagement that cascades through their teams.
How to Build Employee Engagement That Actually Sustains Healthcare Outcomes
Sustainable engagement is not produced by annual surveys or recognition programs alone. It requires a consistent set of management behaviors that positively reinforce the specific actions that drive quality care every day. This is the core principle behind behavior-based performance management.
Behavioral conditions that sustain engagement over time:
- Managers who consistently catch and reinforce the right behaviors, not just correct the wrong ones — an environment where doing great work feels rewarding rather than invisible
- Regular, specific feedback loops that connect individual effort to patient outcomes
- Leadership visibility and accountability that signals engagement is an operational priority, not a once-a-year initiative
Staff need to see how their individual actions connect to care quality. When a nurse receives specific recognition for explaining medication instructions thoroughly and then sees that patient's improved adherence, the behavioral loop reinforces future effort.
ADI's behavior-based methodology — grounded in over 45 years of Applied Behavior Analysis research — gives healthcare leaders a structured way to make this systematic. Using frameworks like Precision Leadership®, managers learn to identify and reinforce the specific behaviors that produce excellent care, rather than waiting for problems to correct. Lasting behavioral change follows.

Organizations that share survey results and involve teams in improvement plans see 23% higher engagement. Leaders must model the behaviors they expect, provide consistent reinforcement, and hold themselves accountable to creating environments where discretionary effort is recognized and rewarded.
Conclusion
Employee engagement in healthcare is not a soft metric—it is a hard driver of the outcomes that define organizational performance: patient satisfaction, safety culture, care quality, and workforce stability.
Its advantages compound over time when built on behavioral consistency. Engaged teams that feel reinforced for excellent work continue to give Discretionary Effort, sustaining improvements rather than reverting to baseline. Conversely, disengagement cascades: it spreads through teams, erodes safety culture, drives costly turnover, and ultimately harms patients.
Healthcare leaders should treat engagement as an ongoing management practice, not a periodic survey event. The behavioral conditions that drive it—consistent positive reinforcement, specific feedback loops, and leadership accountability—are manageable and measurable.
Organizations that build these conditions systematically will outperform those that treat engagement as a secondary concern. The gains are real, the methods are proven, and the science behind them has nearly a century of research behind it.
Frequently Asked Questions
Why is employee engagement important in healthcare?
Employee engagement directly shapes patient outcomes, safety culture, and staff retention. Disengaged employees are less likely to give the extra effort that prevents errors, improves patient satisfaction, and sustains quality care—resulting in measurable harm to patients and organizational performance.
What is employee engagement in healthcare?
Employee engagement is the degree to which clinical and non-clinical staff are emotionally invested and behaviorally committed to their work, their patients, and their organization. It shows up in observable behaviors at the bedside and in care teams, not just in survey responses.
What are the 4 types of employee engagement?
The four dimensions are cognitive, emotional, behavioral, and social. In healthcare, these show up as attentiveness to patient needs, advocacy during handoffs, protocol adherence, and peer support during high-stress shifts — each driven by how deeply staff connect with their work and their organization's mission.
What are the 5 C's of employee engagement?
The 5 C's (Care, Connect, Coach, Contribute, Congratulate) are management practices that build engagement at the team level. In healthcare, they translate into showing genuine concern for staff wellbeing, fostering psychological safety, developing clinical skills, involving staff in improvement decisions, and recognizing behaviors that drive quality outcomes.
How does employee engagement affect patient outcomes?
Engaged employees deliver more attentive, consistent care, which correlates with higher patient satisfaction scores, fewer adverse events, and stronger protocol adherence. Highly engaged organizations are 3x more likely to rank as top performers in patient experience.
What happens when healthcare employees are disengaged?
Disengaged employees underperform on quality metrics, are more likely to leave (1.7x higher turnover risk), and—in active disengagement—can damage team morale, safety reporting culture, and patient experience across an entire unit or department. The financial cost is significant: turnover from non-engaged employees costs healthcare organizations an average of $25 million per year.


